Assault and Great Bodily Injury
In assault and attempted murder cases, a central responsibility is evaluating injury severity to determine whether it meets the legal thresholds for Great Bodily Injury (GBI) or Significant Bodily Injury (SBI). These determinations often shape case outcomes. In some instances, it can be startling to learn that a single punch has led to a fatal injury—underscoring the complexity of trauma assessment.
While the visible injury is important, a comprehensive evaluation must also account for the victim’s medical history and any medications taken prior to the incident. These factors can significantly influence how the body responds to trauma and may help explain why an injury that appears minor ultimately becomes life-threatening.
A structured approach to these cases includes considering key questions:
- How much force was used in the punch?
- Where did the impact occur on the body?
- Did the victim’s blood alcohol content (BAC) influence the outcome?
- What role did the victim’s medical history or pre-existing conditions play?
- What medications was the victim taking at the time of injury?
- Could the victim’s health status have made them more vulnerable to injury or death from a single trauma?
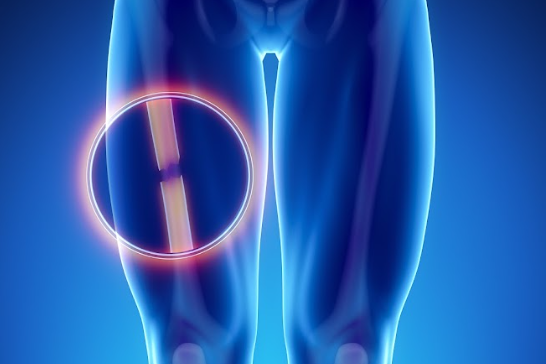
Blunt force trauma occurs when mechanical force—such as a punch or impact with a hard surface—transfers enough kinetic energy to damage the body (Houck, 2017). An object striking the head may result in a traumatic brain injury (TBI), causing disruption in brain function without necessarily producing a skull fracture (Craig Williamson, 2025). Conversely, an impact that causes a loss of balance and a subsequent fall may lead to a subdural hemorrhage—typically associated with acceleration-deceleration forces that tear bridging veins rather than direct fracture—often resulting in more severe long-term consequences (Houck, 2017). These examples highlight that injury severity is not solely dependent on force, but also on anatomical location and vulnerability.
In the context of trauma or assault, injuries may include both hemorrhagic and non-hemorrhagic conditions, such as neurological dysfunction, cardiac dysfunction, mechanical impairment of breathing or circulation, myocardial infarction, and inadequate oxygenation—all of which can progress to shock. “Shock is the leading cause of preventable death in injured patients and is second only to brain injury as the leading cause of death for overall death from trauma” (Christopher Colwell, 2025).
Medications can further complicate outcomes. Individuals taking anticoagulants (e.g., warfarin, heparin, coumadin) and antiplatelet agents (e.g., aspirin, ibuprofen, Motrin) are at increased risk of significant bleeding—not because these drugs initiate bleeding, but because they impair the body’s normal clotting response once bleeding begins (David A. Garcia, 2026).
Alcohol intoxication is also common among trauma patients and presents additional challenges. Acute intoxication can complicate initial assessment and management of injuries, mask critical signs and symptoms, and delay diagnosis (Kathryn Clare Kelley, 2021). Furthermore, alcohol use may impair the body’s healing processes, contributing to poorer outcomes (Does Alcohol Slow Down Healing Bones, Wounds & More, 2026).
Conclusion:
In assault and attempted murder cases, one of the key responsibilities we have is assessing the severity of injuries to determine whether they meet the criteria for Great Bodily Injury (GBI) or Significant Bodily Injury (SBI). These determinations can significantly impact the legal outcome of a case. A thorough evaluation—one that considers mechanism of injury, physiological response, medical history, medications, and substance use—is essential for accurately understanding injury progression and supporting well-informed, evidence-based conclusions.
Works Cited
Christopher Colwell, M. (2025, February 13). Approach to shock in the adult trauma patient. From UptoDate: https://www.uptodate.com/contents/approach-to-shock-in-the-adult-trauma-patient?search=elevated%20blood%20alcohol%20concentration%20and%20bleeding%20&source=search_result&selectedTitle=6~150&usage_type=default&display_rank=6
Craig Williamson, M. M. (2025, December 3). Traumatic brain injury: Epidemeiology, pathology, and classification . From UptoDate: https://www.uptodate.com/contents/traumatic-brain-injury-epidemiology-pathophysiology-and-classification?search=TBI&source=search_result&selectedTitle=2~109&usage_type=default&display_rank=2
David A Garcia, M. C. (2026, March 17). Risks and prevention of bleeding with oral anticoagulants. From UptoDate: https://www.uptodate.com/contents/risks-and-prevention-of-bleeding-with-oral-anticoagulants?search=alcohol%20and%20increased%20bleeding&source=search_result&selectedTitle=2~150&usage_type=default&display_rank=2
Does Alcohol Slow Down Healing Bones, Wounds & More. (2026, March 5). From ScienceSights: https://scienceinsights.org/does-alcohol-slow-down-healing-bones-wounds-more/
Houck, M. (2017). Blunt Injury. Forensic Pathology.
Kathryn Clare Kelley, P. S. (2021, March 27). Impact of blood alcohol concentration on hematologic and serum chemistry parameters in trauma patients: Analysis of data from a high-volume level 1 trauma center. From PubMed Central: https://pmc.ncbi.nlm.nih.gov/articles/PMC8183372/
May’s Open Webinars
Pediatric Strangulation: Not Just “Little Adults” (Back by popular demand!)- Click here to register
Acceptable Medical Practice for Blood Draws- Click here to register
Listening Between the Lines: The Skill and Sensitivity of Child Forensic Interviewing- Click here to register
Pediatric Failure to Thrive: When is it Child Neglect?- Click here to register
Don’t miss our newsletter! Topics covered are:
Assault / Trauma
DUI / General Medical
Child & Elder Abuse / Neglect
Mental Health / Toxicology
Sign up here.