Delirium in criminal cases
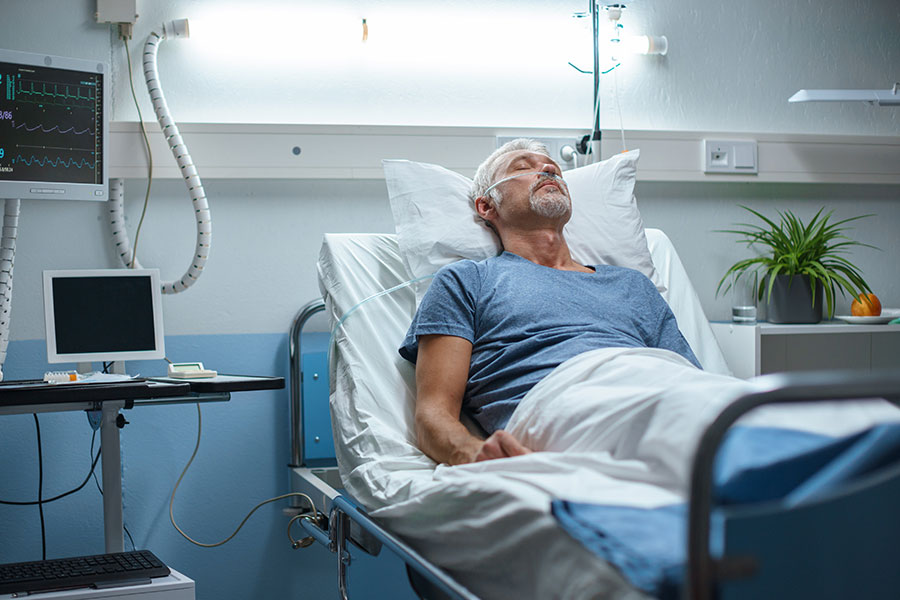
Hypothetically, there is a case where the defendant was injured in a car accident and being cared for the in the ICU. During his hospitalization, he demonstrates bizarre behavior and is diagnosed with a psychotic break. His behavior is presumed to be the cause of the accident and psychiatric care is implemented. A few days later, while having an episode of aggression, he hits a nurse and subsequently gets charged with assault. During the investigation, the family tells the police that they can’t believe it – their beloved uncle is very docile at home with no history of any aggressive or violent tendencies. He would never have hit anyone, much less a nurse caring for him. When questioned, he doesn’t even remember even hitting the nurse.
What is ICU delirium?
Many patients come and go from a hospital on a daily basis, and the majority of them act their normal selves while there. However, the elderly and the patients in the intensive care setting can experience what is called ICU delirium or hospital psychosis. This phenomenon affects approximately one third of the elderly, 80% of ICU patients, and 16-89% of hospitalized patients in general. If this occurs early in the hospitalization, the hospital staff will assume that this is how the patient acts at home as they have never met them before, and this is their first impression. The burden then lies on the family or friends of the patient to communicate effectively with the staff about how the patient acts at home and what is normal and what is abnormal for them. If there is no communication, the delirium will be overlooked as baseline behavior for the patient and therefore will go untreated.
What causes it?
There is not one clear cause of this delirium/psychosis, but many factors contribute to the phenomenon such as surgery, infection, isolation, medication, dehydration, poor nutrition, disruption of the sleep/wake cycle, disorientation, noise, lighting, length of stay. Delirium is defined in The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) as “a reduced ability to direct, focus, sustain, and shift attention, coupled with a change in cognition, in the form of memory deficit, disorientation, or perceptual disturbances.” Risk factors are advanced age, baseline cognitive impairment, increased comorbid disease, frailty, alcohol abuse, drug abuse, and high illness severity. Factors that contribute to the delirium or precipitate it are metabolic disturbances, low blood pressure, sepsis, poor pain control, mechanical ventilation, sleep disturbances, medications such as benzodiazepines or opioids, deep vs. light sedation, anticholinergic medication, steroids, and surgery.
What are the symptoms?
The hospital staff should be on the watch for changes in the patient with symptoms such as shifting attention, incoherence, poor cognition, disorientation, hallucinations, aggressiveness, lethargy, acute changes in mental status, inappropriate speech, inappropriate mood, poor memory, poor conceptual reasoning, anxiety, seizures, tremors, sweating, and/or urinary incontinence. If the condition is not recognized in a timely manner and addressed rapidly, it can lead to increased morbidity and/or mortality. When affected, the patient’s stay in the hospital is usually prolonged due to the delirium and the resulting functional decline. The delirium can last from a couple of days to several weeks or even months. Post-intensive care syndrome (PICS) can develop in these patients and is evidenced by cognitive, psychiatric, and/or physical disability after treatment. Major risk factors of PICS are duration of ICU delirium, acute brain dysfunction (stroke), low blood pressure (sepsis, trauma), hypoxia (cardiac arrest, respiratory distress syndrome), poor glucose regulation, mechanical ventilation, dialysis, and prior cognitive impairment.
What is done to help the patient cope?
Steps can be taken by hospitals to reduce the incidence of delirium, thus shortening the length and severity of the hospital stay and helping the patient to have a better outcome. Some hospitals have emergency rooms dedicated to the elderly and they are trained in detecting delirium. Hospitals may provide staff training on detecting delirium and taking a thorough medical history focusing on mental status. Other accommodations may include daily exercise, ensuring the patient has their hearing aid, and dentures, good nutrition and hydration, promotion of good sleep, encouraging family and friends to visit, and providing familiar objects. Unfortunately, in the ICU setting, a lot of these interventions cannot logistically or reasonably occur. There is a lot of technology surrounding the patient, noises from monitors, beeps, buzzes, machines, suction equipment, other sick people crying and making loud noises, activity such as CPR and procedures being carried out around the clock, and people caring for patients. The ICU is notorious for noise pollution, it is difficult to control and is very stressful.
What is the treatment?
Medications are frequently used when the patient develops delirium/psychosis in order to attempt to control the symptoms. Since surgery and sepsis can lead to an inflammatory response within the brain, steroids and statin medications are being examined as possible ways to stop the inflammation and injury. Haldol, a first generation antipsychotic, has been shown to decrease the duration of the delirium and decrease the development of agitation in the elderly but did not affect the incidence. Risperidone has been shown in some cases to prevent the development of delirium in the elderly population. Dexamethasone, a steroid, was not shown to reduce the incidence or duration of the delirium. Donepezil trials were also unsuccessful. Unfortunately, there is a lack of proven medication to reduce delirium and the side effects of these medications can be significantly negative.
Works Cited
Collier, R. (2012, January 10). Hospital-induced delirium hits hard. CMAJ: Canadian Medical Association Journal, 184(1), 23-24. Retrieved March 1, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3255198/
Hayhurst, C. J., Pandharipande, P. P., & Hughes, C. G. (2016, December). Intensive Care Unit Delirium: A Review of Diagnosis, Prevention, and Treatment. Anesthesiology, 125, 1229-1241. Retrieved March 1, 2021, from https://pubs.asahq.org/anesthesiology/article/125/6/1229/18605/Intensive-Care-Unit-DeliriumA-Review-of-Diagnosis
Luetz, A., Grunow, J. J., Morgeli, R., Rosenthal, M., Weber-Carstens, S., Weiss, B., & Spies, C. (2019). Innovative ICU Solutions to Prevent and Reduce Delirium and Post-Intensive Care Unit Syndrome. Seminars in Respiratory and Critical Care Medicine, 40(5), 673-686. Retrieved March 1, 2021, from https://www.medscape.com/viewarticle/922728_1
Rawal, G., Yadav, S., & Kumar, R. (2017, June). Post-Intensive Care Syndrome: an Overview. Journal of Translational Internal Medicine, 5(2), 90-92. Retrieved March 1, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5506407/
Swift, D. (2019, September 5). Stop Prescribing Antipsychotics for Delirium. Retrieved March 1, 2021, from Medscape: https://www.medscape.com/viewarticle/917787#vp_2
[sep]
Don’t miss our newsletter! Topics covered are:
Assault / Trauma
DUI / General Medical
Child & Elder Abuse / Neglect
Mental Health / Toxicology
Sign up here.