Often in assault or abuse cases, the victim is elderly. When evaluating these cases, it is prudent to retain a medical expert to review the discovery and determine if the injuries are consistent with contusions from trauma or are senile purpura. Contusions (bruises) can have a similar appearance to purpura, but contusions occur because of trauma or physical force to the skin that is either accidental, self-inflicted, or inflicted by another person. Contusions appear as discolored spots that can be painful, oddly shaped, and may have accompanying injuries such as abrasions, fractures, and lacerations. Because of this, it is beneficial if the expert can review the full medical history of the victim, a full history of the incident, and evaluate the photos of the alleged injuries. Unfortunately, many elderly people have dementia or Alzheimer’s disease and are unable to give a thorough medical history or account of the incident, making investigation difficult.
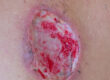
Actinic (Senile) Purpura
This common, benign, connective tissue/skin disorder was initially discovered by Bateman in 1818 and generally affects the elderly population. It is caused by chronic exposure to the sun which causes fragile, damaged skin and manifests as dark purple blotches (macules) and extensive ecchymosis (bruising) on areas of the body that are exposed to the sun on a regular basis such as the hands, forearms, face, legs, and neck. Once the skin is damaged by the sun and becomes fragile, the skin can no longer support the tiny blood vessels that run through it and thus they are easily damaged by even the most minor trauma or shearing force resulting in blood seeping out of these vessels and causing the resulting irregularly shaped blotches. This condition is not painful, tender, or itchy. Upon examination, the clinician will also most likely see other evidence of skin aging such as wrinkles, sallow yellow skin, liver spots (brown, tan or black), rough/scaly areas called actinic keratosis, and or stellate pseudo scars which are white, irregular, and star shaped, along with the actinic purpura. The damage typically lasts from one to three weeks before resolving on its own. However, they continue to recur throughout a person’s life and may cause emotional distress due to the cosmetic damage. Treatment relies on creams and sun protection. It can be found in approximately 12% of people over the age of 50 and up to 30% of people over the age of 75. (Hafsi, Masood, & Badri, Updated 2020 Aug 8)
Imposters
Other diseases or injuries that may present the same way as actinic purpura are as follows:
Steroid-induced Purpura – Topical steroid medication is used for many skin disorders and of course, as any medication, has side effects such as atrophy of the skin, spider veins, stretch marks or striae, stellate pseudo scars (as mentioned above), bruising, infections, acne, rosacea, excessive hair growth, and/or a rash of purple spots known as purpura. This purpura occurs when the protein in the skin degrades leading to fragile skin and thus damage to the tiny blood vessels under the skin. The mechanism causing the damage is different from actinic purpura with the resulting damage causing the same problems. (Abraham & Roga, 2014)
Anticoagulant Usage – A rare condition called warfarin-induced skin necrosis can occur when this blood thinner causes the blood to clot and block the blood vessels, causing an area of destroyed or damaged skin called necrosis. It usually occurs at the beginning of therapy in women more often than men between the ages of 50 and 70. This condition first appears as a painful, purplish bruise-like rash called purpura, progressing to bluish-black with a red rim, blood blisters, and ultimately full thickness skin death. (Vyas & Oakley, 2016)
1. Scurvy – Vitamin C is essential for the development of collagen within the connective tissues of the body, including the skin resulting in fragile skin. If there is a deficiency of vitamin C, a disease called scurvy can develop with symptoms weakness, joint pain, loss of appetite, depression, and purpura. This disease is becoming more prevalent and could possibly be seen in people with various addictions or other causes of malnutrition. (Antonelli, et al., 2018)
2. Vitamin K Deficiency – Vitamin K is essential for blood to clot appropriately, bone health, and vascular health. Various diseases, blood thinning medications, and dietary deficiencies can all cause vitamin K deficiency. A deficiency will manifest itself as a nosebleed, petechiae (brown-purple spots on the skin), a hematoma, bleeding within the gastrointestinal tract, blood in the urine, and/or bleeding gums. (Knott, 2019)
3. Psychogenic Purpura – This is also known as Gardner-Diamond syndrome and is a very rare condition usually seen in women with severe emotional disturbances. First, the person feels fatigue discomfort followed by burning, itching, stinging, and painful skin, anywhere on the body. Next the skin becomes hard followed by a painful, swollen, pink or red raised area. After 48 hours these lesions may turn blue and yellow, becoming less painful. They usually resolve within a week. (Jafferany & Bhattacharya, 2015)
4. Palpable Purpura – These reddish-purple lesions on the skin can be felt and are usually associated with a severe infection of the blood vessels.
5. Primary Systemic Amyloidosis – Abnormal protein build up in the muscles, connective tissue, blood vessel walls, heart, kidneys, and peripheral nerves of the body causing fatigue, weight loss, numbness and tingling, hoarseness, swelling, an enlarged liver, an enlarged tongue, bruising, and petechiae (brown-purple spots). (Nyirady, 2019)
Works Cited
Abraham, A., & Roga, G. (2014, Sep-Oct). Topical Steroid-Damaged Skin. Indian Journal of Dermatology, 59(5), 456-459. doi:https://dx.doi.org/10.4103%2F0019-5154.139872
Antonelli, M., Pecorini, G., Burzo, M. L., Massi, G., Landolfi, R., & Flex, A. (2018, July 22). Scurvy as cause of purpura in the XXI century: a review on this “ancient” disease. Eur Rev Med Pharmacol Sci, 4355-4358. doi:https://doi.org/10.26355/eurrev_201807_15433
Hafsi, W., Masood, S., & Badri, T. (Updated 2020 Aug 8). Actinic Purpura. In S. Publishing, StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK448130/
Jafferany, M., & Bhattacharya, G. (2015). Psychogenic Purpura (Gardner-Diamond Syndrome). The Primary Care Compannion for CNS Disorders, 17(1). doi:https://dx.doi.org/10.4088%2FPCC.14br01697
Knott, L. (2019, February 19). Vitamin K Deficiency. (J. Payne, Editor) Retrieved November 30, 2020, from Patient: https://patient.info/doctor/vitamin-k-deficiency
Nyirady, J. H. (2019, August 5). Primary Systemic Amyloidosis. Retrieved November 30, 2020, from Medscape: https://emedicine.medscape.com/article/1093258-overview
Vyas, R., & Oakley, A. (2016, February). Warfarin-induced skin necrosis. Retrieved November 30, 2020, from DermNet NZ: https://dermnetnz.org/topics/warfarin-induced-skin-necrosis/
Don’t miss our newsletter! Topics covered are:
Assault / Trauma
DUI / General Medical
Child & Elder Abuse / Neglect
Mental Health / Toxicology
Sign up here.