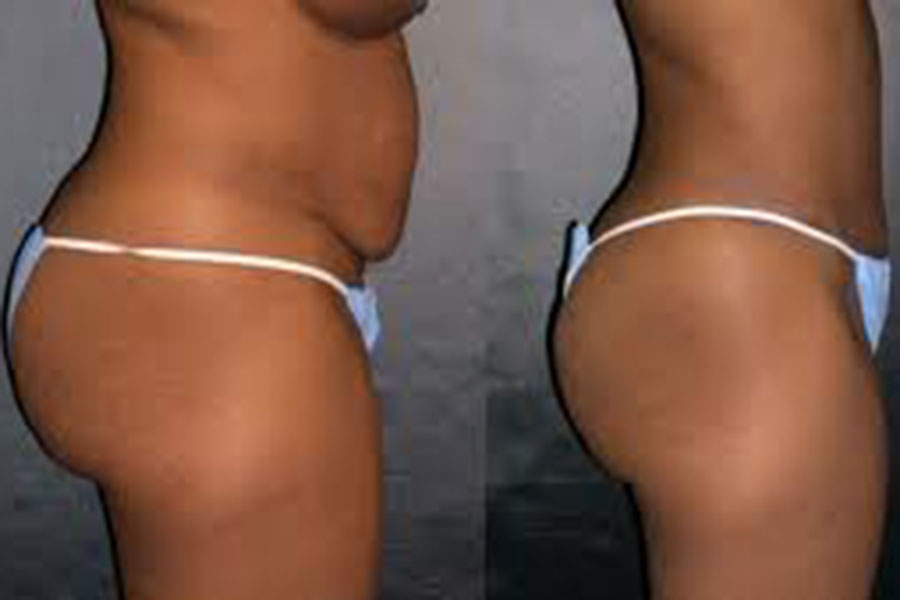
Any surgery carries risk of death, no matter how “routine” the procedure. Any time you submit your body to trauma you run the risk of your body being incapable of handling the additional stress that comes with both the procedure and the healing that follows. Cosmetic surgery has long been on my list of things I don’t agree with. I am fortunate enough to be fairly trim (although we can all stand to lose a few pounds, right?), I am happy with the size of my breasts and nose, I didn’t get horrible stretch marks from bearing my children, and I haven’t had to undergo any procedures which resulted in the loss of a piece of my body other than my appendix and wisdom teeth – which, quite honestly, I can live without replacing. So I definitely will admit that I come from a different place than the people who DO go through cosmetic surgery. And I also have to admit, when I see the before and after photos, liposuction doesn’t seem all that bad!
Now that my disclaimer has been said, I strongly recommend some serious consideration before you decide to undergo any kind of unecessary procedure. This month’s edition of the Journal of Academic Forensic Pathology included a review of the Forensic Implications of Liposuction. In the introduction of the article, the authors indicate that a large majority of people who undergo liposuction are not obese by medical standards, yet they choose to undergo the procedure. Unfortunately, the procedure occasionally results in death. Which goes back to my question “Is it really worth the risk?”
Most the time, when death occurs it is because of infection or clots. Infection is treatable and death in these cases is usually preventable; except in cases where a surgical error results in perforation and severe sepsis. Death from infection is likely due to the lack of proper care provided – either during or after the procedure. The fault may lie on either the patient or the doctor in the latter instance. If the doctor or his staff fails to properly educate the patient on signs and symptoms of infection and when to call the doctor, that is a breach in the standard of care. If the patient knows the risk but fails to communicate symptoms to a doctor or admit themselves to the emergency department, that is the fault of the patient. Clots are a little trickier because they are truly silent killers. In many cases there is no warning and the patient simply dies. Clots are preventable; but putting people on blood thinners is not always necessary and is also not a guarantee against clot formation. Death due to a clot would be much more difficult to prove in a medical malpractice case.
The article discusses several cases in which there was no clear cause of death. In the medical malpractice world this can make the case very difficult to prove. If you don’t know how a person died, how do you know who to blame? This is becoming more and more of an issue as the death rate has increased over the past two decades – most likely due to an increase in the procedure being performed. The unexplained deaths were thought to be a result of medication toxicity or allergy or heart attack due to fluid overload. Sometimes the patient knows they are allergic and fail to notify the doctor, sometimes the information is in the chart and it is ignored. Heart attacks due to fluid overload would require proof from the pathologist to demonstrate the cause of the heart attack. Heart attacks are another tricky area for medical malpractice cases. How can you prove that the doctor knew the patient was at risk for heart attack? Even if the surgery placed undue stress on the heart, it’s not necessarily an area in which a plaintiff’s attorney would be successful. Heart attack and heart failure are known risks of any surgery.
The bottom line is that there is always risk in any procedure and proving a medical malpractice case just because the outcome was unexpected is not always a slam dunk.